Want to know the risks associated with TMS therapy?
It’s normal. That’s why I put this post together for you.
I’ve treated 100’s of patients with TMS therapy over the past 3 years. As a board-certified psychiatrist and chief medical officer of Succcess TMS, I’ve seen it all.
So, what side effects might you experience if you opt for TMS therapy? What are the short and long-term risks associated with TMS?
You’ll find all the answers in this post.
Risks or Side Effects of TMS Therapy?
The vast majority of patients who undergo TMS experience no side effects or very mild ones.
If you do experience a side effect, it’s most likely to be temporary discomfort at the treatment site. Other common side effects include:
- Mild headaches
- Tingling sensation in the scalp, jaw, or face
Most patients who experience one or more of these symptoms find the side effects dissipate in one to two weeks.
Rarely do patients experience anything acutely enough to discontinue treatment sessions.
TMS is non-systemic, which means any side effects are contained in the treatment area and are not widespread throughout the body.
Risks Associated with TMS
Since TMS therapy utilizes a strong magnet, the most notable risk is to those who have any form of metal implanted in or near their head or neck, whether by accident or by design.
Metal in areas that are more than 10cm away from the head is for the most part accepted. Titanium is fine.
Here are some examples of metal in or around your head that might exclude you from TMS treatments:
- Aneurysm clips
- Any medical implant containing metal
- Cochlear implants
- Metal stents
- Shrapnel or bullet fragments
- Tattoos containing magnetic or magnet-sensitive ink
Patient care dictates that no one fitting these criteria is a good candidate for TMS. Pacemakers are fine
The proximity of the metal to the magnetic pulses could cause possibly life-threatening reactions.
If you are uncertain whether you have an implant that could disqualify you from treatment, talk to your doctor.
Long-Term Risks of TMS
You may be wondering whether prolonged exposure to TMS treatment will cause any negative effects down the road.
The FDA has approved TMS treatments for depression and OCD, and clinical studies have been conducted to research long-term TMS risks.
No adverse effects have been associated with long-term TMS therapy.
The magnetic fields utilized in TMS are similar to those in MRIs, but TMS treatment uses only a small fraction of the magnetic field exposure you would experience in an MRI brain scan.
Even if you received several chronic, acute TMS sessions, the total amount of exposure would equal less than a few MRI sessions.
There have not been demonstrated negative effects of repetitive MRIs.
For this same reason, there is no evidence to show TMS can cause brain tumors.
Clinical studies also explored whether long-term magnetic field exposure to TMS therapy can cause memory loss or negative effects on concentration.
None of these systematic evaluations showed any negative impact on memory or concentration.
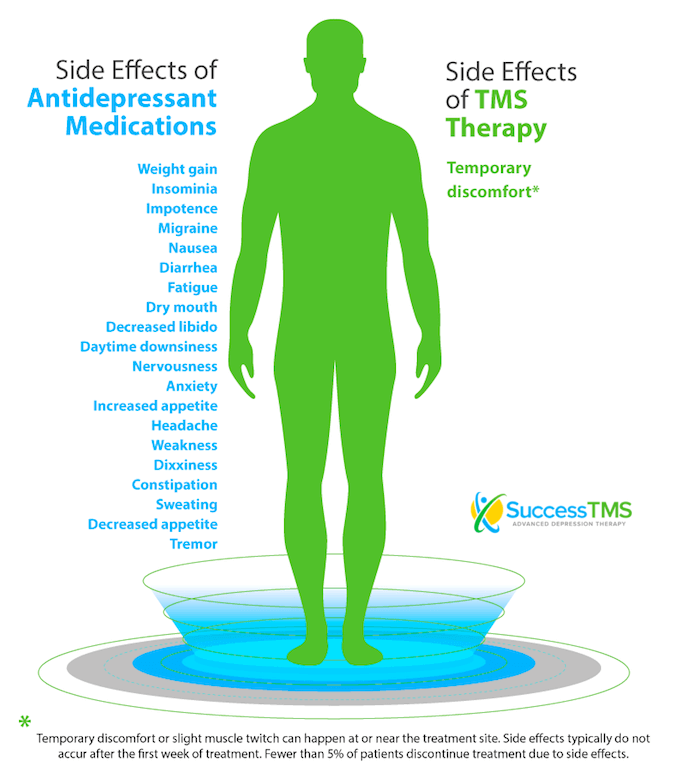
Side Effects of Other Depression Treatments
One major advantage TMS has over other major depression treatments, particularly anti-depressant medications, is its lack of life-altering side effects.
While any negative effects of TMS generally decrease after a patient’s first week of treatment, the side effects of anti-depressants can last through the course of treatment.
They may also worsen as the dosage is increased.
Adverse effects of anti-depressant medications include:
- Weight gain
- Sexual dysfunction
- Gastrointestinal upset
- Dry mouth
- Weight gain
- Sedation
If you’ve tried antidepressant medications to treat your major depression, you’re probably aware of how uncomfortable and frustrating the side effects can be.
Transcranial magnetic stimulation could be a safer treatment option with milder—to no—side effects.
You can find a full comparison of TMS vs medications here.
Get Help Today
It’s time to get help for your depression and anxiety.
Find a TMS treatment clinic near you.
We, Success TMS, are the best-rate TMS providers in the country.
To learn more about how TMS can help you, call us today at 888-406-9648.





51 Comments
I’m just entering my second week of the treatment . I remember after my first session, I was super light headed and feeling like there was nothing inside my head. Then the next couple of days I felt better. Now I feel super agitated after all sessions and headaches persists too.. wondering if TMS is right for me.
Wondering if you continued use of TMS? And if not or so, please let me in. I’m not concidering just yet.
How do you feel now?
I FEEL THE SAME WAY! I’m angry at the littlest things… but half way through the treatment I was at a perfect harmony… I think I was over treated !
Don’t give up Sandra.
First, note if you have changed any of your medications, such as dose changes, missing doses or starting a new medication.
Next, make sure you are well hydrated before AND after your treatments.
Also; it is perfectly fine to premeditate with either Tylenol or ibuprofen or both before treatments if you are prone to headaches. If none of those measures mitigate your symptoms, then it might be a matter of lowering your motor threshold from 120% to 110 or 100% for better tolerability. You still can get benefits from TMS.
If that does not help, then a remapping would be indicated to re-evaluate the coil placement and the pulse strength. TMS still can be a great option for you.
Can this help patients with substance abuse problems?
Yes, there have been studies that are very promising that look at using TMS to treat cravings for various illicit substances, and currently, TMS can be used off-label to treat addiction. Deep TMS with BrainsWay was just FDA approved for treating tobacco smoking addiction. This indication should help pave the way for more research and more FDA-approvals for the use of TMS in addiction.
Does TMS cause agitation? It’s probably not that and just my life right now in general
I felt very edgy my first week of the therapy. I always in the 1-5% group for reactions to things.
Hi CJ,
To answer your question, TMS is not known for causing agitation as a consistent side effect.
You are more likely correct in your assessment, as agitation or irritability is a known symptom of depression.
If you feel your agitation is worsening, perhaps think about what potential triggers might be causing you more frustration lately.
The hope is that TMS can actually help treat the symptoms of depression and give you a better ability to control your reaction to triggers.
Also, sleep deprivation can cause irritability which makes it more difficult to modulate our responses to even what would be a minor stress or trigger.
Make sure you are protecting your sleep while doing your TMS treatments.
Hope this helps.
I’m in my first week of TMS and I feel super agitated. The littlest things set me off. I’m not myself.
It sounds like you are getting activated since starting your TMS treatment.
This can occur sometimes but is usually easily resolved depending on the cause. If you are taking SSRIs or Buproprion, which can be activating medications, then it is possible this in combination with your new TMS treatments can be causing this type of reaction. It may mean your doses can be decreased, but I would recommend you discuss any medication changes with your prescriber.
Also, it could be that the % output of your Motor Threshold (MT) might need to be decreased until you tolerate the treatment better. Usually, the target is 120% of your MT to be therapeutic for treating depression, but you might need to be a little less than that for now.
Speak to your TMS Treater and TMS Provider about what you are experiencing and they can make some possible changes or recommendations to help you tolerate the treatments better.
Hello Caroline,
I am so sorry your son is experiencing these debilitating symptoms.
To answer your questions, yes, TMS can help with OCD.
Deep TMS with the Brainsway system is FDA approved for the treatment of OCD, but the other rTMS systems also have protocols for OCD as well.
The benefits for depression can hold at least 12 months, but some patients do opt to do maintenance treatments as a preventative measure anywhere from 1 treatment per week to 1 per month.
There is not yet sufficient data on how long the benefits for OCD can hold. You are absolutely correct, the nature of the TMS treatments would be great exposure therapy for your son’s intrusive brain tumor thoughts, inherently.
Exposure therapy would be part of the TMS treatments as well, so even visualization of a bridge would be possible. A 50% reduction in OCD symptoms is considered treatment success, and TMS can help him achieve that.
Good luck to you and your son.
I have only had two TMS treatments. First one no problem moved up intensity on the second one caused me to get lightheaded and very tired.
The Tapping is painful
How long to adjust?
Hi Pat,
It is perfectly normal to have some scalp sensitivity early on in TMS treatments.
I highly recommend hydrating well prior to and after your treatments to help prevent the lightheaded feeling as well as headaches.
Also, you can premedicate with any over the counter pain medication such as Tylenol or Advil before your treatments until you get more used to the pulses.
The fatigue you are experiencing is also quite common, especially early on in treatment. It is like your brain is having a “work-out.” It can typically take approximately one week or so to see this improve as you acclimate to your treatments.
Remember to communicate with your treater what sensations you are experiencing during treatment so he or she can make adjustments to get you more comfortable.
Bottom line – it should get better and better as your TMS course goes on.
Good luck to you!
I’m just finishing my first week of TMS. I actually feel more depressed than when I started and the treatments are barely tolerable at 105%. Feels like a jackhammer on the side of my temple and comes out the other temple. Is this normal? I have no scalp sensitivity but it is much more than uncomfortable. They have made adjustments but they are so small it doesn’t really make any difference. I know it’s early in the treatment but I’m doubting if I can . stand having anymore.
Hello Vicki,
To answer your question, it is “normal” to have some sensitivity to the treatments, especially in the first week.
However, the keyword is TOLERABLE.
The pulses should be at least tolerable to you. If over time you are not getting a little better accustomed to the pulses, then let your treater and TMS provider know and they can ReMap you. This would reverify your treatment location as well as your pulse strength that is being used for your treatments.
Drinking a little caffeine before a mapping can help find your motor threshold easier and likely result in a lower pulse strength needed for you.
Also, consider taking an OTC pain reliever before your treatments to help mitigate some of the sensitivity.
Don’t give up. These ideas can help you be able to continue your treatments and get some relief.
Hi Andrea,
TMS is used for depression that does not respond to antidepressants, but it is not limited to refractory depression.
TMS can also be used as an alternative to medication before going down the medication road.
Just note that different insurances have certain criteria regarding past medication attempts which determines coverage for TMS.
I recommend you have a consult with a TMS Coordinator to discuss all options that could work for you.
If you’re near one of our locations call us at 888-406-9648.
Is TMS only an option if you have tried medication without results? Because I don’t want to try medication.
I have had sleep disturbances since 2-3 weeks into my treatments. I am a week out from completing my TMS and I am feeling worse. I can’t sleep at night , I am having trouble with memory and the way my head/brain feels. I suffered a life threatening TBI 35 years ago , with subpar aftercare and just realized a week ago that two of my vertebrae in my neck are fused together…. caused by a traumatic injury. I had to let the medical professionals know that I was having a CFS leak from my right ear….. I’m afraid I have chosen the wrong path
Hello Sam,
I am so sorry you are going through these struggles.
Given your significant history of TBI and now a CSF leak, I highly recommend you follow this up with your neurologist or your primary care physician.
It is possible that the symptoms you are experiencing are either getting exacerbated by TMS or might even be unrelated. Please do not fault yourself for starting TMS therapy. You did nothing wrong; leave no stone unturned.
In light of your current symptoms, you can always pause TMS and revisit treatments when the neurologic issues have been addressed.
It is never too late. Good luck to you.
I am inquiring for my adult son. Wondering what the average time the success stories keep feeling well with OCD (or depression) afterwards. After the 6 week therapy do the results stay the same….. Is there a once a year tune up….. or is to once and done. My son’s OCD makes him obsess over head injuries. He has had concussions and thinks every head bang or headache is a brain tumor. Wondering if this would make him a bad candidate or if he would have a built in exposure!!!!!!! He also has fears of jumping off a bridge so cant drive over them (which would be an impossible exposure)
Do I need a prescription or referral from a psychiatrist, or doctor to get this treatment. Or can i just call and say “ I am depressed and nothing else has worked and I want to try TMS” Am I able to do this on my own?
why does the TMS hurt? it’s very painful, this is my first week. i’m just wondering if this will continue?
The first week of my TMS treatments were very painful. But every day it did get less and less. In the second week I was able to relax and pain was sustantially less.
I have suffered from depression all of my life I have been on many anti depressants with no help. This treatment sounds promising but I have 2 implants in my lower jaw and a plate and screws in my cervical neck. Would I possibly still be a candidate for treatment.
Thank you
Hi Adeline,
To answer your questions, yes, it is not abnormal to have some headaches after starting TMS treatments.
To help this, you can make sure to stay well hydrate, and premedicate with either Tylenol or Motrin before your treatments. That should pass as you get more and more used to the pulses.
Also, if you have depression and anxiety and are doing the depression protocol, then you might be noticing your depression symptoms improving but possibly your anxiety symptoms remaining which causes that to feel more exposed or “worse.”
You should discuss how you are feeling with your TMS provider, as there might be adjustments to your treatment protocol that can help with the chest tightness feeling, such as decreasing slightly your %MT from 120% to 100 or 110. The stimulatory pulses for some people are better tolerated at a slightly lower strength. As you are only on your 5th treatment, be patient with yourself and the process, it might take a little time to get used to the treatments and see results.
Good luck to you!
Hello Cindy,
TMS treatments can cause scalp tenderness while the pulses are emitting.
This sensitivity often improves over time as you get used to the treatments. The key word is that the pulses should be “tolerable” rather than “intolerable.”
It does feel a lot like Woody Wood Pecker tapping on your scalp. You can always take an over the counter pain remedy prior to your treatments.
Talk to your provider if the pain does not improve; your pulse strength might need to be adjusted.
Hope this helps; I encourage you to try to finish the course as it can be very beneficial.
I have had 5 treatments as of today and am experiencing lots of anxiety with chest tightness and headaches. Is this normal and will it subside
Hello Debbie,
I am so glad to hear that you have researched TMS as an option for you.
Given your history of trying multiple antidepressants with little to no benefit, you are an excellent candidate for TMS for that reason.
As for your implants, it does depend on what type of metal you have in your jaw and neck. If titanium, which most surgical procedures use these days, then you should be fine as titanium is a non-ferromagnetic metal and would not be affected by the magnetic coil.
I recommend you first determine what type of metal was used by calling the office of the surgeon and see what is on record of being used for you. Your TMS provider would need to have that information before proceeding with TMS for you.
If you are cleared by your surgeon, then TMS can be a great treatment option for you.
Good Luck!
Hello Alexandra,
The answer to your question is yes, you can, on your own, go see a TMS provider for an evaluation.
That psychiatrist will ask you about your history, the medications and other treatments you have tried for depression to determine if you are a good candidate for TMS therapy.
Many patients coming to my practice are coming “self-referred” after doing their own internet research.
I am so glad that you are empowered to take some control of your depression and reach out for help.
Good luck to you.
test
Will tms help me with my bipolar, bpd, general anxiety, PTSD ? It will make me better or worse right now I’m struggling so bad n the medication isnt helping alot 🙁 I just need something that will help me
Hi Katelyn,
I am sorry you are struggling to get relief from your symptoms with your current medications.
TMS is currently FDA-approved for the treatment of Major Depression Disorder. The other conditions you described are areas of investigation with TMS, but are not FDA-approved conditions. There are many studies that show very good promise with TMS for anxiety disorders and Bipolar disorder.
TMS can help you with those symptoms, but it would be an off-label treatment.
Hey there, I’m just starting TMS for hardcore depression and anxiety … I also have c-PTSD which has a huge overlap in symptoms of bpd and/or bipolar. I’m not a Dr. just a 38year old female. Something that helped me A LOT was the book “The Body Keeps the Score” (do the audio as the book is long) I’ve tried many medications, still struggling bad too. So I’m sorry honey, I feel for you😢The book made me understand why and what ptsd is on a whole other level…Ptsd trauma can’t be pilled away or beaten into submission. The effects of it come out sidesways aka mental health problems that worsen and don’t respond to treatment. did my 2nd TMS today. I know everyone is different but I havnt had any bad side effects. I told the tech to crank it up and today and I’m lethargic. But it might be the answer. I hope you can try it. I’m rooting for us. We deserve to be okay❤️Love and light to you
Hello this is my third week I’m in the 2nd day of my third week I have headaches here and there and sometimes my head feel stuffy and I have some high Anxiety at times I’m still emotional suffering can it be because I’m on clonazepam 0.5mg twice a day and two antidepressants Wellbutrin and Viibryd and how can you tell if TMS is not working for you I’ve been suffering deeply with MDD and BPD and PTSD going on 9 years with no success with medications I’ve been dealing with this for 20 years I don’t want to put my hope into to it and get disappointed cause I’m stuck already can TMS help with this
Hello Thasiha,
I am glad you reached out.
First, you are doing a good thing for yourself with TMS, as your consistency with the daily treatments is the best way to get the best results.
As you are just starting your 3rd week, please do not be discouraged if you are not noticing much change yet.
On average, patients can begin to see changes around week # 2 and #3, but some patients see changes sooner and some see changes towards the end of the treatment course.
Regarding your headaches, that is not an uncommon side effect. Make sure you are well hydrated before and after your treatments and it is fine to take an over the counter pain reliever.
Regarding your anxiety symptoms, it is unlikely to be caused by the clonazepam if you are taking this as prescribed because this is an anti-anxiety medication. Wellbutrin XL and Viibryd can both cause a side effect of activation which feels like anxiety. It is possible both of those medications in combination, though not a dangerous combination, along with your TMS treatments can now be enhancing the activation side effect.
The strength of your treatment pulses might need to be decreased a little to help you tolerate them better, or perhaps the doses of your medications can be adjusted now that you are in your 3rd week of TMS.
I recommend you discuss your symptoms with your TMS provider and the provider who is prescribing your antidepressants.
The take home message for you is that this feeling you are experiencing should be able to be addressed.
Good luck with you treatment.
Currently receiving TMS.
I have headaches on and off for years and now the headaches and sharp pain near the temple are getting worse.
I was asked prior to TMS about concussions and I’ve had approximately 15 over the years.
Just wondering if TMS can have an effect or can make the headache pain worse.
If so should treatment be stopped until a brain scan has been completed
Hello Steve,
First, I would recommend if you haven’t already, let your TMS provider know that you are experiencing headaches with your TMS treatments.
Some people prone to headaches can be more sensitive to the TMS pulses. Your treater might be able to make a slight change with the coil to help, or the provider might change your protocol slightly to see if you tolerate the pulses better.
To help reduce the headaches, you can also take an over the counter pain reliever prior to your treatments. Also, make sure to be well hydrated.
You do not necessarily need to stop your TMS treatments, but I would make sure you let your PCP or neurologist know that you are having ongoing headaches, as they predate your TMS treatments. They can determine if you would need further work-up, like a head CT scan or MRI.
Good luck to you.
I am devastated by the failure of TMS – after 25 treatments I have not responded to the benefit s of TMS I really wanted this treatment to work for me as I’m on multiple antidepressants and was hopeful I could go into remission or even feel better from my chronic depression- but no there has been no result for me which leaves me gutted
Hello Joanne,
I am so sorry you are struggling this way. Please still remain hopeful, because a complete course is 36 treatments and 1/3 of patients are considered “late responders” which means those patients see a noticeable change towards the end of treatment and sometimes even up to 3-4 weeks after treatment ends.
I encourage you to reach out to your TMS provider and inform him or her you feel sick. You might benefit from a remapping to make sure your pulse strength and coil location are still optimal for you. Also, there might be some changes in your protocol that can be made that your depression might respond better to.
Also, studies have shown that people who do it respond to a first course, up to 85 % can respond to a 2nd course, because sometimes 36 treatments is not a magic number.
With all of this in mind, please stay hopeful. You are never out of options.
During treatment my chin shakes, is this normal?
Yes, the pulses can trigger motor movements in the face, much like the pulses made your hand move during the mapping process. If this is uncomfortable to you, adjustments in the coil placement can be made by your TMS Treater or TMS Provider to eliminate or at least decrease this facial muscle response you are experiencing.
I would inform them of this, and see if perhaps a coil angle change can be made first. This simply changes the rotation of the electromagnetic field slightly, but enough to get the pulse of the sensitive spot it is hitting. Another change can be moving the coil a little more towards the front of your face, to better move away from the motor strip of your brain cortex.
This is typically not a dangerous reaction, but it can be annoying, so please speak up about it to your TMS team.
It took a long time for my doctor to find the right spot to get an impulse in my hand. I’m worried the pulses are not directed where they need to be. How critical is precise mapping?
This is a very good question.
The target area is about the size of a quarter, so there is a little wiggle room. However, it is important to be as accurate as possible for the best possible results.
You wrote it took a while to find an impulse in your hand. This should be more specifically your thumb where the twitch should be found for the most precise location. If a twitch in your whole hand was found and not a particular finger, then you might want to request a remapping from your provider.
The difference between finding a twitch in your ring finger and your thumb can be important in finding locating your target site based on your own brain anatomy.
Is TMS an option if I’ve had a cavity filled? The old style filling, with metal. Not the new ceramic/polymer cavity fillings.
Yes, metal dental fillings are considered safe with TMS.
I have both depression and anxiety. I’ve heard that bilateral rTMS is sometimes used in this case. With coil placement on the right to lower anxiety (with lower pulse to reduce activity???), and coil placement on the left to decrease depression (with higher pulse rate). Is this common, if so how successful is this type of practice? Any details appreciated. I’m currently getting dTMS over the left DLPFC and it is making me more anxious and doing nothing for my depression.
First, I am so glad you are trying TMS for your depression and anxiety.
To answer your question, yes, “bilateral” rTMS has been used to treat Depression and target anxiety more directly, however, you need to be aware that the right-sided low-frequency pulse is considered an off-label protocol, as anxiety is not an FDA-approved indication for TMS at this time.
The deep TMS system actually has a broader pulse range, and can target both the left and right DLPFC, however, for some patients, they can tolerate the rTMS system better with less activation, which is what it sounds like you may be experiencing.
Without knowing how far into your treatment course, it is difficult to make any suggestions. If you are early on in your treatment course, it is not uncommon for this activation to occur and then subside.
I recommend you discuss the symptoms you are experiencing with your TMS provider and see if any changes need to be made.
I have received approximately 25 TMS treatments and have experienced a remarkable decrease in my depression! One thing that I have noticed over the last few weeks, though, is that I have had greater fatigue during the day. I haven’t seen any documentation of this being related to TMS therapy, so was wondering if this could be related, or if I may need to decrease the dosages of my antidepressants. I am currently on Lamotrigine 200mg every am and pm and Nortriptyline 50mg every pm. I know I will need to consult with my psychiatrist, but was just wondering what the standard is concerning this. I am also on other meds for my migraines etc that I was wondering if these dosages usually need to be adjusted after this therapy as well. Thank you!
That is so wonderful that you are feeling relief from your depression symptoms since starting your TMS course!
It is actually not uncommon for patients to report some fatigue maybe a few hours after treatment; think of TMS like a “work-out” for the brain. Usually, this phenomenon occurs early on in the TMS course and goes away over time. If you are feeling fatigue some time after your treatment, the first thing to try is moving your treatment session time to later in the day, that way the fatigue is timed a little better for you, more in the evening.
Also, it is true that many patients are able to decrease doses of medications as a result of responding well to TMS treatment. You are on relatively low doses of both medications you listed in your comment, but it is something for sure to discuss with your psychiatric prescriber.
If you are noticing less migraines, then it is possible your migraine medications can be adjusted as well.